Strengthening Financial Control with Unified Claims & Benefits Administration

Where Operational Execution and Enterprise Governance Converge
Claims administration is where operational performance becomes most visible. It is also where financial exposure becomes most measurable.
Every claim reflects the integrity of upstream data, benefit configuration, eligibility governance, and reimbursement logic. When these elements are fragmented across systems, inconsistencies surface in adjudication, payment accuracy, and reporting transparency.
Claims environments do not operate in isolation. They amplify whatever discipline — or disorder — exists upstream.
The Hidden Cost of Fragmented Claims Ecosystems
In many health and voluntary benefits environments, claims systems operate separately from benefit configuration and eligibility governance. When these domains are not aligned, organizations encounter persistent friction, including:
-
High volumes of manual claim review
-
Inconsistent application of benefit rules
-
Accumulator reconciliation challenges
-
Payment delays and rework
-
Limited financial visibility across adjudication outcomes
Manual intervention becomes normalized. Exception handling increases. Administrative overhead grows.
More critically, financial predictability weakens.
When benefit logic and claims execution operate across disconnected systems, even small configuration discrepancies can introduce payment inaccuracies or compliance risk. Over time, this erodes provider and member trust and increases operational scrutiny.
Why Claims Modernization Matters
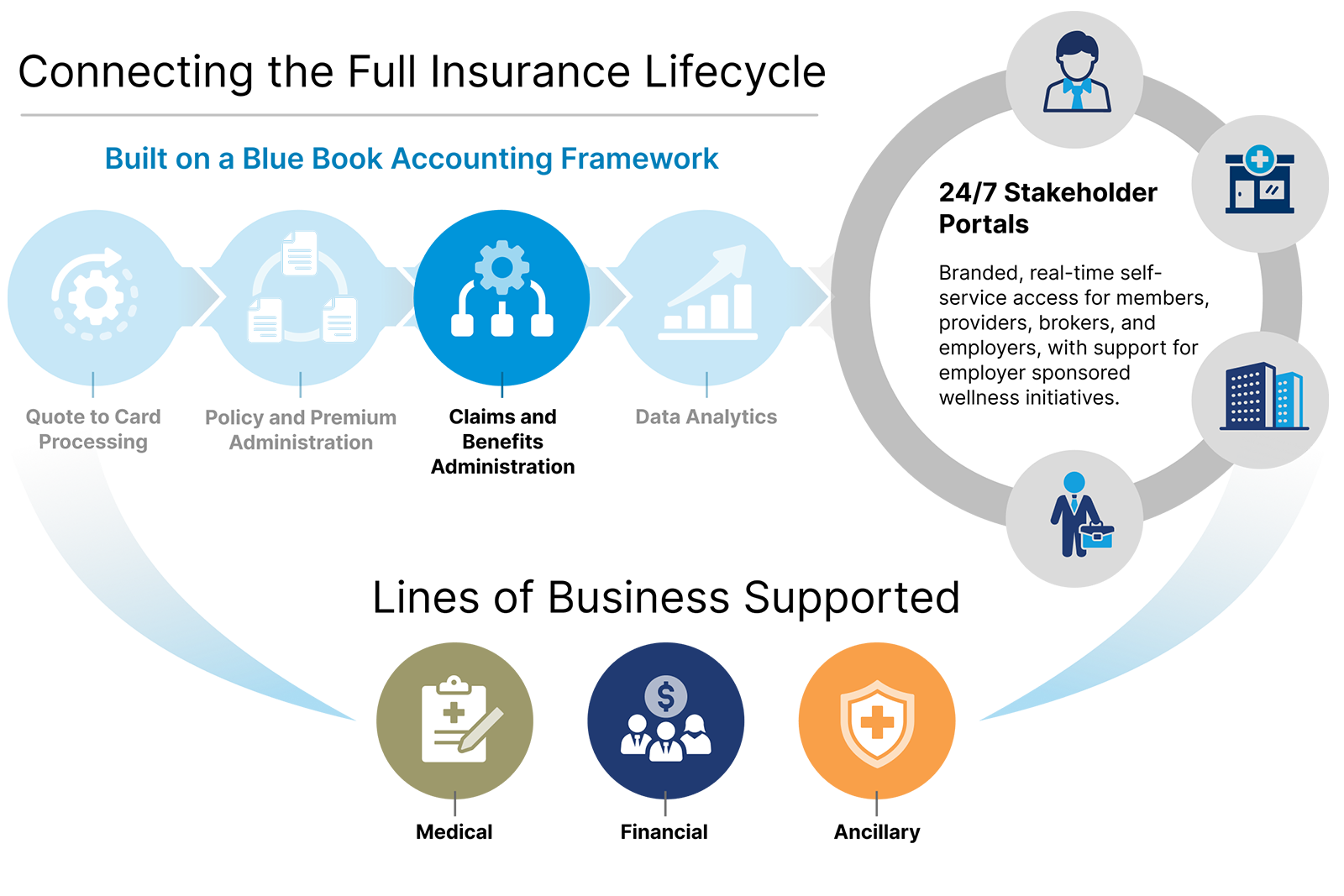
Modernizing claims is not simply about accelerating adjudication speed. It is about aligning benefit governance and payment execution within one controlled enterprise framework.
Unified claims and benefits administration improves:
-
Adjudication consistency
-
Reimbursement accuracy
-
Financial reporting integrity
-
Operational transparency
When claims logic, eligibility validation, and benefit configuration are centrally governed, organizations reduce reactive corrections and strengthen enterprise control.
Claims modernization becomes a governance initiative — not just a processing upgrade.
Modernizing Claims with EbixEnterprise
EbixEnterprise Unified Claims & Benefits Administration centralizes adjudication, benefit configuration, and financial controls within a connected enterprise environment.
Rather than managing claims workflows separately from policy governance and eligibility logic,EbixEnterprise aligns these domains within one operational architecture.
Capabilities include:
-
Automated adjudication workflows
-
Configurable benefit and reimbursement rules
-
Integrated accumulators and eligibility validation
-
Payment processing with embedded financial controls
-
Direct alignment with policy, billing, and analytics modules
By unifying benefit governance and claims execution, organizations reduce manual review, improve reimbursement accuracy, and strengthen oversight across the payment lifecycle.
Because EbixEnterprise Claims Administration operates within the broader EbixEnterprise ecosystem, eligibility data, rate logic, and benefit structures remain consistent from policy through payment.
This continuity improves automation rates and enhances financial predictability.

From Processing Efficiency to Financial Governance
Health and voluntary benefits organizations operate under increasing pressure to control cost while maintaining service quality. Claims administration sits at the intersection of those priorities.
Fragmented claims environments often force organizations into reactive management — correcting discrepancies after adjudication rather than preventing them at configuration.
Unified claims modernization within EbixEnterprise shifts that model toward proactive governance.
Organizations gain:
-
Greater payment accuracy
-
Stronger compliance oversight
-
Reduced administrative overhead
-
Improved provider and stakeholder confidence
Modernization at the claims layer strengthens both operational execution and enterprise financial control.
Within the broader EbixEnterprise modernization framework, EbixEnterprise Claims Administration represents a powerful entry point for organizations prioritizing governance, efficiency, and reimbursement integrity.
Back to EbixEnterprise Insurance CycleLearn More
To explore how EbixEnterprise can help your organization achieve digital transformation, contact:
Mark Brown
Vice President, Sales
Ebix Health Division
mark.brown@Ebix.com